It wasn't intended to be a comprehensive discussion of mental health issues by any stretch, but I wanted to at least mention some of the more common issues we encounter as paediatricians. Obviously every topic I spoke about is worthy of a talk in its own right, but hopefully this will have made people think a little bit and generated some useful discussion.
***Trigger warning*** Discussion of self harm, suicide and eating disorders.
"When I was first asked to give this talk, I had two reservations. The first - would anyone want to hear a grand round from such a junior member of the team? That was dealt with pretty swiftly, with assurances that training level didn’t matter so long as content was good. Hopefully that’s something I can achieve. The second, however, was more of an issue. Would people actually want to listen to a talk on adolescent mental health? The answer to that was less positive. In fact, it was a resounding “no”. And I think that's part of the problem, and it's exactly why I decided I should give this talk.
How do you feel about your patient now? Don't focus on what you think the differential is, think about your reactions and feelings towards this patient. Are they wasting your time? Are you less inclined to take their other complaints seriously? Are they an attention seeker? This may sound dramatic, but we're all guilty at times of responding negatively towards issues such as deliberate self harm.
There are lots of different ways in which I could represent the distress caused by mental illness, but I think one of the most effective is to share the story of a young person I've been involved with, including some of her quotes.
Suzie is 15. She presents to her GP after being encouraged
to attend by her form tutor. The consultation is difficult. After some
encouragement, she says that has been experiencing low mood for the past 3
years. She does not feel she has any friends. She feels that she is
unattractive and is not achieving at school. Her eye contact is poor and she
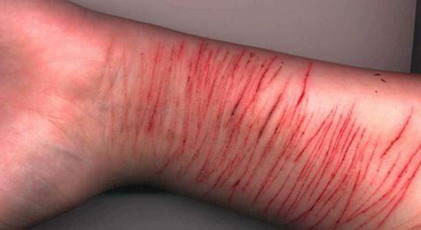
has a blunted affect. On examination, she appears well. Some superficial
lacerations are noted over her thighs and forearms.
This encounter is one Suzie still feels uncomfortable about.
“I was pretty cross that I’d been made to see a doctor. It’s hard enough for
people to get appointments without me taking them up. I actually felt quite
guilty about using a slot which could have been given to someone who was
actually ill. I was also really worried about admitting I cut myself. It seemed
like people felt that that was something done for attention, so I wanted to
hide it as much as I could; I didn’t want to be seen as an attention-seeker
when actually I just did it to try to feel better.”
Suzie is referred to CAMHS, who commence an SSRI and offer
CBT, which she declines.
Suzie vividly recalls her CAMHS appointment. “I was 15 and
it was the Christmas holidays. The department was located in an old, probably
Victorian, terraced house which hadn't been particularly well renovated. The
room I was seen in was freezing. There were two people seeing me; a middle aged
lady who was a social worker and a younger man who introduced himself as a
"trainee doctor" - I suspect that he was a psychiatry registrar but
at the time I was pretty convinced he was a medical student. They sat behind a
desk for the whole consultation and the seats for us (my parents were with me)
were a good few metres away from them. There was also a little window at the
top of the wall where someone else was apparently watching what was going on.
On the wall were several posters about how to deal with your child's difficult
behaviour and advising against smacking. There were toys all over the floor.
My first impression was that they thought I was a child
(which of course I was, at least legally, but what 15 year old doesn't think
they're incredibly grown up?). I don't recall much of the discussion we had. I
remember them repeatedly asking whether I'd ever been abused, and then later
taking great delight in asking my parents to leave the room so that they could
ask me again. Actually I only wanted my parents out of the room because I knew
they'd be upset if they knew the extent of my depression, but the doctor and
social worker seemed pretty desperate to uncover some horrific trauma which
must have caused my problems.
I didn't go back after that first appointment. They put me
on fluoxetine. They also wanted me to have CBT but I declined. In retrospect, I
probably should have gone for it, but at the time the only time I could cope
with being "mental" was to tell myself and everyone else around me
that it was due to "a chemical imbalance in my brain". Taking
medication to correct this was fine. To have CBT would have been admitting that
my thinking was fundamentally flawed and that it was therefore some weakness of
character resulting in my problems and not a "proper" illness. Of
course I know now that that isn't true, but the explanation I got was such that
that was what I believed at the time.”
Shortly after commencing treatment, Suzie attempts suicide
by taking 64 paracetamol tablets.
Even now, Suzie finds it difficult to articulate exactly why
she tried to end her life. “I was fed up of everything. Nothing I did seemed to
have any point. I didn’t think I’d ever achieve anything. I saw how unhappy my
Mum was, knowing I felt like this, and that made me feel incredibly guilty. I
was sure I was making my whole family miserable and that without me there,
they’d all be better off. I could just about believe that they might be
initially upset if I died, but I really felt that they’d get over that and be
far happier than they could with me around. I wanted to stop feeling miserable
and I wanted to stop dragging other people down with me.”
Suzie recovers from her suicide attempt with no residual
physical effects. She continues to self-harm by cutting herself with razor
blades. In addition, she begins to struggle with food, going through periods of
severe restriction followed by binges. She often induces vomiting and abuses
laxatives.
Although diagnosed with bulimia, Suzie feels that her eating
behaviour was closely linked with her mood. “Food made me feel better when not
a lot else did, but after I'd stuffed myself senseless I'd feel so guilty and
dirty that I'd have to make myself vomit... Some days, I just didn’t feel like
I’d possibly emptied my stomach, so I started taking laxatives too. I knew it
was dangerous but I didn’t care. I felt that I’d rather die than put weight on.
Sometimes, after a purge, I didn’t feel the need to cut myself as much. It was
like the vomiting was a kind of release, in the way that cutting was.”
Although all cases are very different, this is a fairly typical case. But so what?
What does this matter? What's the impact of self harm? Well, there is evidence to suggest that in young people like Suzie, who self-harm, risk of premature death is considerably higher than in the general population. Whilst, unsurprisingly, risk of completed suicide is up to 25 times higher than those who don’t self-harm, risk of accidental death is seven times and death from natural causes twice as high as the general population. Mean years of life lost was over 25 for both males and females (Bergen et al., Lancet 2012). Self-harm is also associated with poorer educational and employment outcomes, increased risk of mental health problems and increased risk of substance misuse in later life (Mars et al., BMJ 2014). The UK has one of the highest rates of self-harm in Europe (at
400 episodes per 100 000 population) (Hawton et al, Lancet
2012)
So what can we do about it? How can it be treated? Although self-harm within itself is not a diagnosis, the majority of young people who self harm will have an affective disorder, most commonly depression, although anxiety, eating disorders and psychotic disorders such as schizophrenia may also occur. The only licensed anti-depressant for under 18s is
fluoxetine. Paroxetine (Seroxat) in particular has been linked with increased risk of
self-harm and suicide after initiation of therapy, but there is some risk with
all anti-depressants. There are multiple theories as to why this is, but it may
be to do with returning energy levels and drive once treatment is commenced.
It's therefore important to ensure that any young person commenced on anti-depressant therapy have regular follow-up and support. The evidence base for any therapy is limited, although psychological therapies
are being increasingly developed and investigated.The current recommendation is that moderate-severe depression is treated with a combination of an SSRI and CBT, although resources mean that this isn't always available.
There are a number of reasons why people attempt suicide.
Life stressors, such as financial worries and relationship breakdowns are
particularly common precipitators, as are psychiatric symptoms. However, many
people who attempt suicide do not realise that their symptoms are due to an
illness (Lim et al., Journal of
Affective Disorders, 2014). This is important because it means that the first time people present to medical services will be with a suicide attempt. They often won't seek help for their underlying psychiatric symptoms because they don't realise they have an illness which can be treated. Over 10% of young people experience suicidal
ideation and around 4% will attempt suicide at some point before the age of 25.
Suicide is the third commonest cause of death in 10-24 year olds. Suicide
attempts are more common in girls and those with a diagnosis of depression (Grudnikoff
et al., European Journal of Child and
Adolescent Psychiatry, 2014).
Eating disorders are a huge topic and obviously worthy of a whole talk within themselves. However, I felt it was worth mentioning them because they commonly co-exist with affective
disorders. One study found that 18.5% of patients referred for anxiety or
depression had problematic eating, with 7.3% met the diagnostic criteria for an
eating disorder, with those who were younger, female and having a history of
self-harm most likely to be affected (Fursland and Watson, Eating Disorders,
2013). It's therefore important that we are know to look out for these things, because anorexia nervosa in particular has a high mortality rate.
So, what can we do about this? Well, they key is to listen. A recent report published by the Royal College of Psychiatrists, and endorsed by our royal college, the RCPCH, suggests that simply listening and taking a sensitive history has therapeutic benefit. Groups such as Cello and Young Minds, who do a lot of work with young people affected by these issues, find again and again that doctors do not feel comfortable dealing with mental health issues in young people. They do not feel they have the necessary skills to help and they don't know what they're supposed to do. However, the evidence shows that actually, something as simple as just talking about the issue in a sensitive way helps. We all have the skills to take an history and listen to someone. It isn't difficult or complicated, yet it helps to reinforce a positive image of healthcare services in a young person's mind and means they are more likely to engage with services in the future.
That's been a brief overview of adolescent mental health issues. Hopefully it's made you think about how you might deal with these issues, and reinforced that all of us have skills which will help us to deal with them.
I don't usually put references at the end of blogs, but in case anyone is interested, these are some of the papers I read whilst I was preparing this talk.
BERGEN, H., HAWTON, K., WATERS, K.,
NESS, J., COOPER, J., STEEG, S. and KAPUR, N., 2012. Premature death after
self-harm: A multicentre cohort study. The Lancet, 380(9853), pp. 1568-1574.
CELLO, YOUNG MINDS,
2012. Talking Taboos: Talking Self Harm. Cello Group
FURSLAND, A. and WATSON, H.J., 2014.
Eating disorders: A hidden phenomenon in outpatient mental health?
International Journal of Eating Disorders, 47(4), pp. 422-425.
GRUDNIKOFF, E., SOTO, E.C.,
FREDERICKSON, A., BIRNBAUM, M.L., SAITO, E., DICKER, R., KANE, J.M. and
CORRELL, C.U., 2014. Suicidality and hospitalization as cause and
outcome of pediatric psychiatric emergency room visits.
European Child and Adolescent Psychiatry, .
HAWTON, K., SAUNDERS, K.E.A. and
O'CONNOR, R.C., 2012. Self-harm and suicide in adolescents. The Lancet,
379(9834), pp. 2373-2382.
LIM, M., KIM, S.-., NAM, Y.-., MOON,
E., YU, J., LEE, S., CHANG, J.S., JHOO, J.-., CHA, B., CHOI, J.-., AHN, Y.M.,
HA, K., KIM, J., JEON, H.J. and PARK, J.-., 2014. Reasons for desiring death:
Examining causative factors of suicide attempters treated in emergency rooms in
Korea. Journal of affective disorders, 168, pp. 349-356.
MARS, B., HERON, J., CRANE, C.,
HAWTON, K., LEWIS, G., MACLEOD, J., TILLING, K. and GUNNELL, D., 2014. Clinical
and social outcomes of adolescent self harm: Population based birth cohort
study. BMJ (Online), 349.
ROYAL COLLEGE Of PSYCHIATRISTS,
2014).Managing Deliberate Self-Harm in Young People (College Report CR 194).
Royal College of Psychiatrists


No comments:
Post a Comment
And how does that make you feel?